- Aug 17, 2020
What keeps pregnant women from attending care?
What keeps pregnant women from attending care? What are the reasons for their late enrolment in antenatal care? Which factors would increase skilled birth attendance?
What keeps pregnant women from attending care? What are the reasons for their late enrolment in antenatal care? Which factors would increase skilled birth attendance?
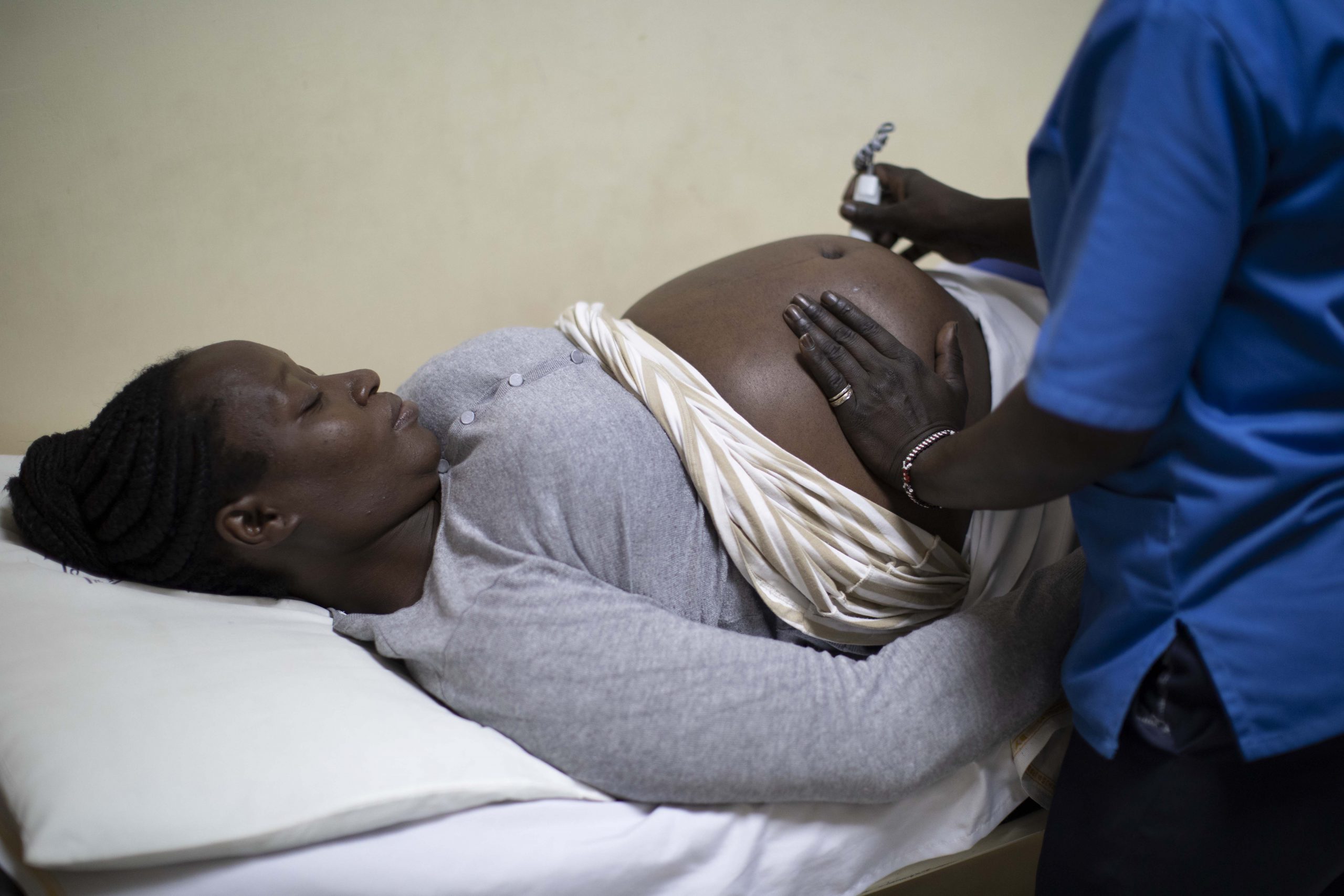
This study seeks to answer these questions using data from more than 1,500 pregnant women enrolled in the MomCare program in Nairobi, Kisumu, and Kakamega counties in Kenya. It assesses patterns of adherence to antenatal care (ANC), and identifies key challenges in attending ANC visits and skilled delivery. Moreover, it offers insights for the design of more effective antenatal care interventions in the future.
Antenatal care is a critical factor in reducing complications and death ratios for mothers and infants during the maternal journey. However, the costs of high-quality antenatal care are an obstacle to seeking care for many women in Sub-Saharan Africa [1]. Additionally, pregnant women often prefer to postpone their first ANC visit as long as possible, which leaves them at a greater risk of developing unnoticed complications. Moreover, coverage of skilled birth attendants in 2018 was only 59 percent in Sub-Saharan Africa, further contributing to the consistently high maternal and infant mortality rates.
In Kenya alone, more than 6,000 maternal deaths, and 35,000 stillbirths occur each year [2]. In fact, the maternal mortality rate in Kenya is 139 percent higher than the average of lower-middle-income countries [3][4]. With a well-functioning health system, most of these deaths would be avoidable. Predictions show that nearly 160,000 more newborn lives could be saved in Sub-Saharan Africa if 90 percent of women received ANC instead of the current 69 percent [5].
To eliminate these preventable deaths, PharmAccess Foundation initiated MomCare in November 2017 to support pregnant women and providers of maternity care. MomCare mainly incentivizes ‘adherence to care’-journeys through a digitally-enabled smart contract. MomCare enrolls pregnant women in a partly or fully subsidized health insurance program and offers them a ‘health wallet’ on their mobile phone which they can use to check-in and pay at the clinic. The health wallet runs on a mobile platform that enables sending nudges, reminders for check-ups and rewards to patients to improve their adherence to care, while simultaneously rewarding providers financially for quality care provision when women complete their journey.